(A repost from my old blog, 24 and 26 May 2009)
PART ONE
I’m afraid that, shot up with babble-juice, I subjected some of my brave and noble visitors at the hospital to more detail than they really wanted. I wasn’t complaining, but in addition to being powerfully unpleasant, my stay at the hospital was really quite interesting in some ways. In my drug-addled state, I was geeking out on how surgery had changed since my last experience with it in 1992. So thank you, visitors; I hope you will forgive me because your presence there certainly helped me.
Geeking out on all the medical stuff
Anyway, a small subset of people have expressed actual geeky interest in the gory details, and since my mind is clearing up for increasingly long periods now (about a half-hour out of every three that I’m awake) I’ll write them here. What follows has been typed up in small installments over three days, when I am coherent enough.
Consider yourself warned, everyone else; if you would rather not know, skip this post and the one following. This is all about the squishy stuff.
I’m just middle-aged if I plan to live to a hundred and four, but it isn’t like I ever grew up in the first place. Physically I’m overweight but very active; seldom drive, bike most everywhere in all seasons, never take the elevator, etc. I do strength-training, sit in a chair without a back, lift weights at my desk. This is no virtue; I have a chronic muscle pain condition that only responds to exercise, so I do it constantly. Have always joked about my unhealthy diet; exercise covers a multitude of sins, doesn’t it?
Not necessarily.
Never get medical checkups
The day (Friday) before it happened, I was in my doctor’s office for a routine checkup. We had some concerns and he scheduled me for tests on Monday, including a CAT scan that would certainly have found the failing diverticula along with the thing it was looking for. You see what happens? Go to the doctor, next day you’re courting the grim reaper. It isn’t worth it.
That afternoon we had a graduation celebration at the college where I work. I rode my unicycle into a few people’s offices to visit, helped myself to the grille, just enjoyed the festivities. That evening, I came back to campus to ride around on my uni including a couple assaults on the steep ramp along the South side of Milner library. That is some heavy-duty exertion for a guy my size, and something didn’t feel quite right in my gut. I shrugged it off; a guy my age has no business eating bratwurst. Or at least not a bratwurst, a burger, some potato salad, some chips, an apple, a Diet Coke and a cookie.
A beautiful afternoon on my birthday
Then Saturday, my birthday, about two ‘o-clock Diane and I were riding on the Constitution Trail to visit our favorite bike shop’s open-house. The shop has new owners, a really great couple. It was a beautiful sunny day, there were kids on unicycles, people with every kind of cycling interest, free bratwurst on the grille, bag-tosses, sales, etc. Big doors wide open, lots of high-end stuff out for drooling over. Diane was looking at helmets and I was looking at a cutaway carbon mountain bike frame, marveling at how light and rigid it was.
In the space of about ten minutes, “something not quite right in my gut” had developed into kidney-stone level pain. Left side, down low, it could be an old hernia repair that gives me trouble sometimes. Didn’t feel like a stone, though, and when I used the shop’s bathroom there was no blood in my urine. Diane confirmed for me that the pain was nowhere near my appendix.
“Ride home, get the car, and come get me,” I said. My bike won’t easily fit in her car, but the shop owner agreed to store it for me.
Denial ain’t just a river in Egypt
This is the part where it gets embarrassing. I’m having major abdominal pain, so I told Diane to take me right from the bike shop to the hospital, right? Nope; I wishfully thought it must be some kind of gas pain, or bowel spasms and that it would “pass”. I wasn’t going to spend four thousand bucks on a false alarm, no sir! Never mind that every other time I’ve had that level of pain, it turned out to be something really serious, so I asked her to take me home. (A little hint, darling; your man is only semi-rational most of the time. Torturous pain throws that right out the window and I can rationalize anything; gas pains, a survivable apocalypse, voting Republican, anything.)
In the ER
That afternoon I sweated through waves of pain, hoping for that holy bowel movement or whatever that would save me. Eventually Diane went to bed and slept soundly. About 1:30 am, a glimmer of common sense appeared in my mind and I realized I had to wake her up.
Only problem was, she wouldn’t wake up. I spoke loudly, nudged her shoulder, turned on the light. Went downstairs and posted on my blog, then came back upstairs and called in the nuclear option: I wiggled her toe. She bolted upright, gasping for breath. “What?!!”
It was graduation night: as we entered the ER a young man in a tux was being led away handcuffed by police. I wondered if it would be a good deal to cosmically trade his troubles with mine. We joked with the nurse who checked us in about frequent customer credits and maybe getting my ‘regular room’.
I told them “no blood in the urine” but for some strange reason they declined to take my word for it. Then they mounted an IV, took blood samples, and gave me a shot of liquid courage. The middle-aged male nurse, a man “built like me”, joked about hospital gown designs. No obvious reason appeared (or they were eliminating everything but the least-wanted diagnosis) and an order for a CAT scan was given.
CAT stands for Computed Axial Tomography and it’s basically a spinning x-ray machine that assembles the “slices” in a 3-dimensional image that shows a lot more than a regular x-ray. It’s the next best thing to exploratory surgery, without all the blood and dramatic music. This CAT had been internally upgraded since the last two times I’d used it. It only takes a couple minutes to do a scan.
While I was away getting scanned Diane heard someone say; “52-year-old male, time of death, 3:14 am”. She bolted to the door and listened more intently. In the distance, she heard me cough. Oh, well some other 52-year-old male then.
We waited 30 minutes while the radiologist and doctor looked at my virtual innards. The doctor came in and delivered the news: perforated colon. “We’ve called in the surgeon, Dr. W., and she’s on her way.”
I didn’t even know this Dr. W., who was on call on a Saturday night. The nurse confided: “She’s really good. I hear people speak very highly of her all the time.” That helped me calm down a bit. But when we were alone I asked Diane; check this doctor out. Wide awake? Careless? Sober?
A perforated colon isn’t a case of wait-and-see; bowel material has escaped into the abdominal cavity. Usually the victim will die quite unpleasantly unless action is taken right away. I wasn’t sure what operation was needed though. Maybe something minimally invasive, fashionably laproscopic?
Heh.
Dr. W. came into the room and right away I felt better. Here it was just past three in the morning, and her hair was straight, her lipstick straight, and she had a clear-headed way about her that few people achieve at midday. In crisp, logical fashion she described the problem, range of possibilities, possible fatal and nonfatal complications, and the likely outcome. When I woke up, I’d probably have a colostomy bag for several months, then need another, smaller operation to tidy up. Yes, you can ride a bike with a colostomy bag; people do everything with them. No, she couldn’t say when I’d recover; “I haven’t even done the surgery yet.” Yes, it would be OK to attempt a bowel movement before the operation, but it wouldn’t change her procedure or the outcome.
She asked what medicines I take – everybody asked that. I must have told twenty people that I take a multivitamin, some flaxseed oil (for Omega-3) and aspirin every day. Aspirin’s the miracle drug, isn’t it?
Her voice sounded pained. “Why do you take aspirin every day?”
My neurologist told me to, after my last head injury. To prevent stroke.
Her words were measured and precise as she repeated; “Your neurologist told you to take aspirin everyday.” Apparently neurologists and thoracic surgeons do not routinely compare notes.
(I later realized where I’d seen that exact facial expression and tone of voice: in the movie Jurassic Park where the paleontologist Alan Grant turns to the geneticist and says incredulously; “You bred raptors.”)
Going into surgery, and the panic attack
I’m not a panicky kind of guy. I have literally put out fires without breaking unrelated conversations. I once looked at my mangled hand after an accident and thought; “Oh good, the adducting tendons are still attached.” I’ve had abdominal surgery before.
It was beginning to dawn on me that this would not be an easy laproscopic procedure with a quick recovery. Sign here, and here, and – do you want your parts back like Mister Goodwrench? No? Sign here. Can we let students watch the operation? Sign here. Can we put you in restraints if needed? Sign here. On and on went the consent questions; you know you’ll probably have a colostomy? Sign here. Give your watch and eyeglasses to your wife.
All this while my terror was growing. They covered me in hot blankets and wheeled me down the hall, down another hall, up an elevator, and into the surgical ward.
The table was incredibly narrow, and had towels stacked up on it to be convex so I’d be arched backwards. I was starting to breathe faster and faster. My head was way back, pinching my neck. Could I have a pillow, please, some head support? Someone lifted my head a bit. The soft rubbery oxygen mask was pressed on my face; a tight seal around my nose and mouth. I tried to inhale: no air!
I flailed, I pushed. Can’t breathe! Someone held the mask just away from my face; tears streamed down the sides of my head into my ears as I began to hyperventilate. It was the last thing I remembered.
PART TWO Warning: Pure medical geekery follows
As I said before, though my hospital stay wasn’t any fun, it was very interesting. Lots of gadgets, new procedures, ways to not kill patients. This (very long) post will deal with some icky stuff, so you might want to skip it unless you find that kind of thing as interesting as I do.
I was plenty scared about the anesthesia among other things. You don’t have to read very many sensational news articles about people being awake but paralyzed during surgery for it to play on your fears. Fortunately (to say the least) that didn’t happen.
Anesthesia has really improved. In the past, waking has been like fighting through a swamp, wandering this way and that to find a way out of a dark maze. But this time I woke up easily in a large room somewhere, my mind pretty clear right away. That’s a neat trick considering what I had just been drugged into ignoring only an hour previously.
Well not entirely clear. Someone said to me; “Welcome back, Mister Wiman.” (all smiles) “You didn’t get a colostomy!” Great. I wondered: where am I, and what’s a colostomy? But only a couple minutes later I had sorted that out and was fully awake and damn glad not to have one. Story continues below the fold, with photos.
Gut-wrenching: the actual operation, what little I understand about it
What is a perforated bowel? It’s a hole in the large intestine that allows bowel material to escape into the abdominal cavity. When this happens you need surgery NOW. My perforation was in the sigmoid colon. I received a twelve-inch vertical abdominal incision, and the operation took three hours, roughly twice as long as expected. The incision was closed with about 45 surgistaples.
I wasn’t able to find any videos of this type of operation being performed, or even any good pictures, but that may be just as well. From what I’ve been able to find out the surgeon has to lift out your guts, rinse them off and lay them alongside, rinse out the abdominal cavity, inspect and repair the guts, and pack them back into the abdominal cavity. Do they practice origami in medical school? (If anyone with medical training can provide a more accurate description, I’d love to improve this post with it).
Post-op killers, considered
Clearly the medical community has made an effort to address some of the big ones. These include infection, drug dispensing errors, blood clots from the legs, and fluid buildup in the lungs.
Respiration: Suck On This
Fluid tends to build up in post-op patients’ lungs, often with fatal results. There are several, painfully simple reasons for this. A person who has just had abdominal surgery doesn’t like to cough OR even to breathe deeply. It’s uncomfortable! Another, when lying in a hospital bed, breathing is shallow because you are at rest.
The solution is for the patient to breathe deeply many times an hour, but telling them to “breathe deeply” is pretty vague. So I was given a simple “incentive spirometer”, which is a little plastic flow-meter invented for asthma patients, that lets me know exactly if I was breathing deeply enough. I was told to use it ten times an hour for every hour I was awake, and given specific volume goals. It’s simple, cheap and effective if you can get the patient to cooperate, which I did. It’s not like I had anything else to do.
Move, dammit! And self-managed pain control.
Patients used to be kept very still following surgery (or even childbirth). They were supposed to “rest”, which made for poor circulation, shallow respiration, and the formation of adhesions between abdominal layers. Now we’re advised to get out of bed as soon as possible after the surgery. Get off that bed and walk! My first walk, with someone helping, was from my room to the exit sign down the hall and back. After five days I’d figured out that the hallway circumference of the recovery wing was about 400 feet, give or take. One day, all told, I racked up nearly a mile over several walks pushing my own IV pole the whole way.
This is where self-managed pain control is crucial. They WANT you to use the morphine. It was very funny how several people took the time for a detailed description of how to operate the morphine pump. (C’mon, folks; I’ve used them before and it only has one button.) Dr. W. said; “We want you to move, we want you to cough. You won’t do either if it hurts.”
To sleep, perchance to dream (forget it, big boy)
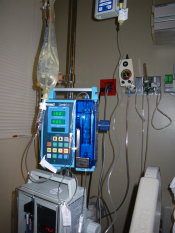
This is a non-trivial problem and they didn’t seem to have a very good handle on it. Every one of the six (!) tubes connected to my body was an opportunity to wake me up and do something to them at regular, overlapping intervals. In fact, the IV tube split off to multiple sources, which drained into me in sequence partly by gravity order (clever, that) and partly by computer control.
They were constantly checking my vitals too (and a good thing, because my blood pressure really spiked at one point). Charting involved waking me up to scan my wrist band, and ask me my name and date of birth to make sure they were not about to give me someone else’s drugz. There was too much light and noise, and of course, I was very uncomfortable. I didn’t get more than an hour’s continuous sleep for nine days; between sleep deprivation and drugs I literally could not track the passage of time. I got online a couple times but nothing made sense to me. I’m still coming back but the important thing is; you have a better chance of sleeping at home.
(UPDATE: I forgot to mention the hallucinations. Drugs plus lack of sleep meant I was hallucinating whenever anyone was not in the room. Patterns in the wallpaper became evil faces, judging me. I was… glad for visitors.)
You really do need this kind of oversight after major surgery, so I can’t think of a ready solution.
The nine-day massage
A major cause of post-op deaths and stroke is blood clots from the legs. I woke up to find that a pneumatic device was squeezing my calf muscles at one-minute intervals, essentially pumping blood through my legs. I’m told most people don’t like this machine but I loved it! Because of my chronic pain condition, sitting or lying still for more than a few hours is a terror to me. But this machine prevented the pain and here’s the cool part: if I can find a portable version, I’ll be able to travel by air again. Several helpful people (including my boss) did some research and found that there are indeed portable versions of these machines. Some time this summer I will be acquiring one, and here I didn’t even know they existed. If there is any silver lining to the whole experience, this is it.
The hand grenade and mega-weirdness
There was a tube protruding from the side of my abdomen ending in a little silicone rubber bulb the size of an orange. They called it; “the hand grenade” and its purpose was to collect drainage from my abdominal cavity. The tube was sutured to my abdomen, which was very uncomfortable. Every few hours, they’d come empty the hand grenade into a cup, measuring and inspecting the resulting fluid. Once emptied, they’d sqeeze it concave and then cap it, to maintain negative static pressure relative to the abdomen.
It was kind of a frightening little device, and when Dr. W. finally snipped the suture and pulled out the tube (which was about two feet in length) I could feel it sliding past my innards as it came out. Ugh!
Stomach pump and why I’m grateful for something I hated so much
I woke with a tube in my nose that ended in my stomach, connected to a stomach pump. I’d munch an ice chip, and a few moments later the little bit of water would hop the u-turn at my nostril and head for the pump. This was in place because the intestines wake up at different rates, and at first anything in the stomach would result in vomiting. As this is the first surgery I’ve ever had where I didn’t vomit (thank doG!), it was a very good thing.
But also a bad thing. I can hardly describe how unpleasant it is to have a tube down the back of your throat from your nose. It’s like (and is) having a giant glob of snot back there which you cannot expel in any way whatever. When after 40 hours the tube was finally removed – like all tubes a long steady pull with weird feelings as it slid past internal parts – it was nearly three feet long. Apparently they want it to coil and lay at rest in the stomach, rather than poking the lining. I stacked up five tissues, reared back and blew my nose, an action which has never felt so wonderful before. Context is everything, I suppose.
Foley Catheter and mega-weirdness
This is the third time I’ve been ‘cathed’ and it isn’t my favorite thing in the universe to say the least. Several years ago following a hernia operation, my urethra or prostate clamped down and I couldn’t pee. The nurse said helpfully; “If you don’t pee, I’m going to have to cathe you!” They waited a very long time until I was excruciatingly uncomfortable (your bladder can literally rupture) before inserting the tube into my penis up into the bladder to relieve the pressure.
This time and one of the other times, the Foley was inserted while I was unconscious, which is worth asking for, if circumstances allow. On a previous occasion (kidney stone requiring surgery) I had a Foley for six days, and it permanently damaged my urethra. Like the cartoon character Hank Hill, “I have a narrow urethra!” This one stayed in for five days, but seems to have left no ill effects. Very, very weird when pulled out-and like all the other tubes, disturbingly long.
Farts and surreality
Sometimes it felt like I’d awakened in a Salvador Dali painting. Beautiful, young professional women would enter my room and ask; “Hello Mister Wiman! Have you passed any gas today?” We joked about what it would be like if other businesses inquired of their customers about this bit of information. “Hello, welcome to Sears! Have you passed gas today?”
But it’s a really important, even crucial question. After all that rough handling, the intestines shut down and there’s no peristalsis. Until every section from stomach to anus starts functioning, you can have nothing by mouth – it would back up and you’d vomit. The OK signal is repeated farting.
“What part of ‘nothing by mouth’ did you not understand?”
Recently I’d been thinking about experimenting with fasting. I’d read an abstract of a study that found fasting one day every two weeks improved insulin response in overweight individuals. Well I got my experiment: for seven days I had no food or drink by mouth at all. My IV tube provided only electrolytes and glucose. I’d question Dr. W. (who really didn’t mind using sarcasm, which I appreciated) about this and she’d say; “No, really, it’s OK! You can just not eat for a week and it won’t hurt you.” Or at least, hurt you less than the alternative. She said; “We’ve had people who are very hungry lie about passing gas, then vomit and aspirate, and end up in ICU on a ventilator. It’s an unfamiliar circumstance to them so they need to understand what it means.” I told her I was only irrational, not stupid. Jury still out, perhaps.
Staples; not just for the office anymore
What can I say about staple stitches? They certainly worked well but I was industrial-strength curious what it would feel like to have them removed. “Oh, it doesn’t hurt at all – it just pinches a bit,” said the nurses. That should have been my first warning.
My skin is super-sensitive to pain. When possible, I take my own stitches out, chilling the area with an ice cube first. I couldn’t reach these so the nurse cooled them with an ice pack and took them out with a clever little pair of special pliers. As it happened, these hurt like crazy. I basically screamed like a nine-year-old girl. Sorry, but ice packs aren’t cold enough, so if there’s ever a next time (perish the thought) I’m insisting on direct ice cube preparation. Apparently for many people, it’s no big deal.
Full incision image available by request. Trust me, you don’t want it.
Next installment; a hospital is no place to get better.